Legalization of Cannabis in Canada
The use of cannabis for medical purposes has been legal in Canada since 2001 and access to medicinal cannabis is currently governed under the Access to Cannabis for Medical Purposes Regulations (ACMPR). As a response to a ruling of the Federal Court of Canada’s regarding the Allard v. Canada case, the ACMPR replaces the former Marihuana for Medical Purposes Regulations (MMPR), which were in effect from March 31, 2014 to August 24, 2016. Prior to the MMPR, access to cannabis for medical purposes was authorized under the Marihuana Medical Access Regulations (MMAR), which came into effect in 2001 and was repealed in 2014.
The federal government has indicated its intent to legalize, strictly regulate and restrict access to marijuana for recreational purposes; and is expected to introduce new legislation in the spring of 2017 following an extensive consultation process.
Doctors for Responsible Access has thoughtfully considered the many issues related to the use of cannabis for both medical and recreational purposes and has established a set of principles that support its ultimate aim, that is to protect the health of Canadians, and especially at risk populations such as youth.
These principles include the following:
- That there are both significant benefits and harms associated with the use of cannabis and further research is required.
- That traditional research models may be too limiting and not easily applicable to Cannabis. Other models need to be considered as the medical profession and regulators seek to establish evidence-based guidelines, policies and standards.
- That technology based solutions are required to reduce the administrative burdens experienced by cannabis practitioners and patients, and to better enable ongoing evaluation and research.
- That a public health approach encompassing both medical and recreational use of cannabis is required.
- That physician support, education and involvement are crucial if physicians are to be part of the solution, ultimately protecting public health.
- That access to cannabis by at-risk populations should include additional requirements or restrictions aimed at reducing risk (for example, mandatory education or smaller quantities for youth under 25 years of age).
- That regulations and solutions must be realistic and practical, if they are to be effective. They must be able to evolve as new evidence emerges and the legal and socio-political environments continue to shift.
Canada has one of the highest ratesMore than 40% of Canadians having used cannabis in their lifetime. Canadian youth are the top users of marijuana in the developed world according to a 2013 UNICEF Office of Research report. (28% vs 5.5% in Sweden). It is estimated that 3% of Ontario’s high school students use cannabis daily of cannabis use in the world, especially among its youth. Although there are potential benefits to the use of cannabis, we still do not fully understand the side effects, potential harms and long term impacts. We also are unaware how cannabis compares to standard formulations of approved cannabinoids such as Nabilone or Dronabinol. Because of the risks, we believe legalization should include measures to strictly limit access and enable large scale research, allowing critical questions of effectiveness and potential side effects to be answered.
Non-standardized black-market cannabis cannot be a substitute for licensed prescription drugs when we seek to undertake clinical research. Canada is in a privileged position as all medical cannabis patients have access to standardized formulations with known concentrations of active ingredients, a prerequisite for robust clinical research.
We are now well beyond the prohibition era discourse that considered cannabis as simply a criminal justice issue. Our children live in an age when cannabis was and always will be readily available, socially tolerated and a largely acceptable form of self-medication for a variety of conditions. We share the concerns and support the conclusions brought forward by the Canadian Center on Substance Abuse (CCSA). Other organizations have also voiced their concerns on cannabis policy, such as:
- Drug Policy Futures
- CAMH (Centre for Addiction and Mental Health)
- SAM (Smart Approaches to Marijuana)
- The Canadian Public Health Association
- CRCR (Council on Responsible Cannabis Regulation)
- Doctors for Cannabis Regulation, and othershttp://www.leap.cc/, http://ssdp.org/, http://cssdp.org/, http://www.drugpolicy.org/, https://www.mpp.org/, http://norml.ca/, http://goo.gl/W5ncJV
Many organizations have even proposed very specific measures, such as the “First Time 5” campaign for the purpose of educating novice cannabis users.
Doctors for Responsible Access is advocating for an approach aimed at the reduction of cannabis-related harm, and diversion of cannabis to youth, as important priorities. We also believe our medical associations should include more physicians with medical cannabis expertise when drafting regulations, guidelines and best practice standards.
“The perception that cannabis is a safe drug is a mistaken reaction to a past history of exaggeration of its health risks”
– Wayne Hall
The risk of legalization is that we run the risk of sending “the wrong message”:
- That cannabis is safe and harmlessMaking it more available to adults — even if restrictions are in place — will increase the access for teens. Just the campaigns to legalize marijuana can have the effect of persuading adolescents that marijuana is not dangerous, which can have a devastating impact on their lifelong health and development. - Seth D. Ammerman, MD, member of the American Academy of Pediatrics Committee on Substance Abuse and cannabis related harms are either greatly exaggerated or negligible and can easily be dealt with later as they arise. This projection, reinforced by several favorable studies on cannabis related harms, encourages a very liberal approach where personal freedom and convenience play a major role on the desired outcome of legalization.
A tight access mechanism would send “the right message”:
- That the risks from cannabis and the new high potency concentrates are still largely unknown and need to be researched, that use can lead to great harms, and access to vulnerable populations such as youth and people with a history of mental illness“Efforts to prevent, reduce or delay the use of cannabis—especially among youth who are particularly susceptible to the risks posed by cannabis—could result in decreased rates of mental health disorders, saving unnecessary suffering and costs to the healthcare system.” -CCSA: Clearing the Smoke on Cannabis, April 2015 should be controlled and supervised. This approach recognizes the uncertain outcome of greater normalization of cannabis and encourages a cautious and stepwise introduction supported by evidence.
Doctors are divided on the issue:
The medical profession is splintered on the issue of medical cannabis. A 2012 study by the Canadian Medical Association (CMA) showed that 64% of physicians surveyed were concerned that patients who request medical marijuana may actually be using it for recreational purposes. The CMA also believes there is insufficient evidence to support its use for clinical purposes. Legalization for recreational use has polarized physicians even further. Even among those who acknowledge the medical benefits of cannabisCannabis contains nearly 500 different compounds, for which we have little or no knowledge of their effects. There may even be complex interactions between the various compounds which produce an “entourage effect”. We still are unsure exactly how cannabis affects the growing mind, but research may one day give us clearer answers. Interestingly, the complex chemical signature of cannabis makes it easily traceable through forensic analysis, as long as the source material is systematically tested. and prescribe it to their patients, many still don’t agree with the idea of adding yet another potential public health risk to the list along with alcohol, tobacco, and opioid abuse.Cannabis is a unique substance with no equal in modern society and we believe legalization should be considered independently from alcohol and tobacco. Parallels between these drugs are inaccurate on many levels and should be avoided as they tend to add confusion to the debate. For example, the effects of one or two consumptions of alcohol wears off quickly whereas the effect of cannabis will leave someone under the influence for the rest of the day and have subtle effects that can last for weeks. We’ve known for decades or centuries the long term negative impacts of tobacco or alcohol, the word is still out when it comes to cannabis. It will take decades of data collection to ascertain the true impacts of the dried plant and the plethora of recent high potency concentrates. All we know is the damage is more insidious than alcohol and tobacco, and has gone by relatively unnoticed, since no deaths have been directly attributed to acute intoxication. Subtle brain damage never make headline news. Others view legalization as the most sensible solution to reducing the disproportionate harms of criminalization and expect negligible long term public health consequences.
There seems to be a general consensus that personal cannabis possession and use should not be penalized with severe criminal consequences. Doctors for Responsible Access shares this view but we maintain that legalization comes with the added risk of normalizing this drug and potentially increasing its use.
The evidence?
While there is a growing international body of evidence, cannabis has only recently been studied in small clinical trials and shown to be effective in treating several medical conditions. However, by the standards of traditional controlled drug trials, the level of evidence still does not reach an acceptable level for clinical recommendations, and there have been conflicting results.
Furthermore, many conditions listed on Health Canada’s Marihuana for Medical Purposes Regulations (MMPR) document are based on anecdotal evidence and this has created a peculiar dilemma for physicians. While we are permitted to prescribe cannabis for these unproven conditions, this practice is quite contrary to the evidence-based paradigm and our medical associations are unable to provide proper guidance as a result.
Gatekeeper’s role: is this medical or recreational?
As physicians who also prescribe medical cannabis, our first-hand experience with this powerful drug gives us a unique perspective. While we may be convinced of the medical value of cannabis and its related compounds for certain conditions, we remain concerned about the lack of clinical research, guidance and regulatory oversight. We are also concerned that cannabis is being prescribed by some practitioners for conditions where there are known risks, such as for pregnant women.
A study published in 2016 indicated that 86% of people who report ever using cannabis for medical purposes also use it recreationally. Calling something “medical” doesn’t always mean it is. As physicians, we face the gatekeeper’s dilemmaIn Canada, nearly 50,000 patients are authorized medical cannabis users but it is estimated that up to 500,000 self-report using cannabis for various medical reasons. In Colorado alone, over 300,000 requests have been registered since medical cannabis was legalized over certain patients’ recreational motives or those that resist trying conventional treatments for their condition. We also witness unpredictable side effects, have to deal with the risk of dependence and counsel patients who have suffered the sometimes catastrophic consequences of cannabis use disorder. In this context, Doctors for Responsible Access feels compelled to caution the authorities to take a very prudent approach.
Under the Access to Cannabis for Medical Purposes Regulations (ACMPR), prescribing cannabis in Canada continues to be up to the individual physician’s knowledge, skills and judgement.
And while Health Canada suggests limiting medical cannabis for a small number of conditions, such as HIV related illnesses and multiple sclerosis, the endocannabinoid system has been shown to play a role in a long list of other conditions including diabetes, cancer, atherosclerosis, ADHD, anxiety, Alzheimer’s disease, and schizophrenia. However, cannabis is not currently the generally accepted treatment option for most of those conditions at this time.
Left without adequate guidance by our medical associations, many physicians feel uncomfortable with medical cannabis and refuse to prescribe it to their patients, while others have seized this opportunity and are exploring uncharted territoriesIn Montana in 2014, 10 doctors wrote 90% of the State’s cannabis recommendations, and one of them wrote 40% by himself. In Arizona, 24 doctors wrote 75% of all recommendations.
We at Doctors for Responsible Access believe in the middle path, where patients should be granted easier access to medical cannabis for a limited number of conditions and for clinical trials after proper screening and evaluation.
Cannabis is not a first-line treatment for any medical condition at the present time. Our approach would allow for large scale clinical research that will help to determine its true therapeutic potential.
There is another set of challenges facing physicians as gatekeepers. The existing regulations for access to cannabis for medicinal purposes impose significant administrative burdens upon physicians, patients and providers. While controls are absolutely essential, when the controls become so burdensome, they dissuade patients from accessing medical grade cannabis through legitimate channels and effectively encourage them to obtain cannabis from black market sources, without the assurance of quality and safety. Some physicians are also imposing additional fees upon patients to help cover the administrative costs. For these reasons, Doctors for Responsible Access believes that we need to make better use of technology to reduce the administrative burden, while also collecting data that can be used for research purposes.
Waiting for the evidence (and guidelines):
Physicians have many concerns when contemplating cannabis as medicine. The pain-reducing and calming effects of THC and its related compounds are often accompanied by many unpredictable individual responses that range from anxiety and paranoia to euphoria or a trance-like state. Presently, we must acknowledge that we are not the experts. Decades of prohibition has pushed clinical research into the hands of patients, producers and a few daring holistic practitioners. While their courage needs to be respected, we need to take this anecdotal knowledge and apply the rigours of clinical research in order to maximize benefits and minimize harm.
In the interest of patient care, we need to be open to considering the best evidence that does exist, and to use that evidence to inform our treatment decisions for each patient. The risks associated with cannabis use differ vastly for a dying patient experiencing extreme pain and discomfort, and a pregnant woman experiencing nausea.
The hurdles we face are manya. convince our medical associations to get actively involved with medical and recreational cannabis and the related public health issues
b. analyze the pertinent scientific data
c. identify the right conditions to treat
d. take into account our patients’ other illnesses and medications
e. weigh the risk vs benefits
f. determine the optimal dose
g. determine the best route(s) of administration
h. persuade patients to use standardized formulations such as capsules, suppositories and mucosal sprays
i. negotiate with patients who will prefer smoking or vaping the dried cannabis plant with unpredictable pharmacodynamics and pharmacokinetics
j. determine the best way to monitor and adjust the treatment regimen
k. expect a wide variety of possible side effects
l. face the possibility of dependence and find strategies to best deal with this outcome
m. and finally deal with the administrative burdens that come with a non recognized treatment
as our medical associations have distanced themselvesThe Canadian Medical Association states there is insufficient data on the safety and efficacy of medical cannabis. The American Medical Association and the American Academy of Pediatrics clearly oppose cannabis legalization. The American Academy of Neurology (AAN) doesn't advocate for the legalization of medical cannabis to treat neurologic conditions because of the lack of evidence. The American Academy of Ophthalmology doesn’t find any benefit in using cannabis for glaucoma. from these issues.
At Doctors for Responsible Access, we believe physicians need to get involved in this debate and in a balanced and sensible way. We also need to enter into dialogue with our patients. We can choose to ignore the reality of cannabis and its use, but many of our patients will not. They will explore and self-medicate with or without our approval, support or guidance.
Cannabis and the developing brain.
Increased use and diversion will inevitably increase cannabis-related harmsAlthough cannabis‐related harm is mainly concentrated among a limited sub‐group of users who use cannabis heavily and/or began to use it at an early age, there are major concerns regarding the potential long term outcomes of cannabis legalization with people who suffer from mental health disorders. Although causality has not yet been determined, it has been estimated that frequent cannabis users have between 50% and 200% increased risk of psychosis and that higher potency (THC) cannabis places users at higher risk of mental health problem. For those patients with cannabis dependence, 61% have a co-existing mood disorder and 45% have an anxiety disorder. 31% of patients with schizophrenia consume cannabis. Patients with schizophrenia who used marijuana are twice as likely as nonusers to take medicine incorrectly or not at all, and six times as likely to dropout of treatment altogether. Cannabis and traffic accidents: Although no deaths have been reported to be caused directly by cannabis, over 4000 or 12% of traffic fatalities are associated to cannabis in the U.S. each year. The issue of its effects on the developing brain has received much attention, and the consensus is far from being reached. There is growing evidence that early cannabis use can have pronounced and permanent effects on the developing brainThe human body’s own cannabinoid system is very complex and plays a crucial role in the the developing mind. It delicately modulates communications between neurons, strengthens or weakens certain connections, and encourages neuron formation. This process is completed at approximately the age of 25 and there is growing scientific data that tends to support the hypothesis that regular cannabis use before this age may leave permanent yet subtle brain damage. If we want to get cannabis legalization right, this is probably the single most important factor we need to take into consideration.. This riska.) Regular heavy marijuana use for teens can lead to a drop in IQ score of up to eight points.
b.) Adolescents who begin cannabis use before age sixteen perform significantly worse on neurocognitive tests than those who start using it later and were more than twice as likely as nonusers to drop out of high school.
c.) Substance-abusing teenagers who cut down their use of alcohol or other drugs went to school more often. This also held true for marijuana abusers, but only if they quit entirely.
d.) Teenagers who smoke cannabis will more likely abuse alcohol as adults
e.) 87% of people who end up with a cannabis problem started using before age 17 may be unique to cannabis, but studies show conflicting results. One study involving twins has put into question the direct role of cannabis and suggests other factors that could explain the cognitive decline in adolescents.
We believe it is imperative to settle this matter but research using non-standardized black-market cannabis will not permit us to resolve the issue. Cannabis products have rapidly evolved over the last few decades and now contain very high concentrations of THC and little or no CBD, another cannabinoid found in the plant which may (or may not) have protective effects. Getting to the bottom of this debate should be a priority but will take large cohorts of users to determine the safety profile (if any) of different strains.
Early initiation and frequent usea.) Youth between the ages of 15-24 years consume three times more Cannabis than adults over 25 years, making it the largest potential target market.
b.) Children who use cannabis are four times as likely as adults to become chronic heavy users, the type to generate consistent sales for the cannabis industry.
c.) Cannabis dependence occurs in 9% of users when started in adulthood but can occur up to 17% of those who begin using it in adolescence.
d.) In a survey in 2014 by the International Journal of Drug Policy, 10% of high school students said they did not consume cannabis but would if it were legal
e.) Legalizing cannabis won’t cure alcohol abuse. While it seems hopeful to believe that legalization will encourage substitution from alcohol to cannabis and reduce harms, research has shown that problematic cannabis users are most likely to have an alcohol problem as well.
are the two main factors associated with long term harm from cannabis. The prevalence of cannabis dependence is twice as high for those who begin using it in adolescence (17% vs 9% for adults) and as perceived riskPublic opinion on the relative safety of cannabis may seem positive for the time being, but it is not a clear indicator of future risk. Cocaine was perceived mostly as a trendy club drug in the 70s and early 80s. That opinion changed overnight when an All American college basketball star died of an overdose in 1986. Negative perception by high school students doubled and use dropped by two thirds and has remained relatively steady ever since. No school-based education drug program could claim to have as much success. It took a tragedy to change public opinion. Acute intoxication with cannabis edibles has recently been associated with unexplainable suicides in the United States but since no deaths have been attributed to direct intoxication, we find ourselves faced with an insidious future threat. of cannabis by teenagers has been steadily dropping in the polls since the 1990s, the message we send with legalization will have a direct influence on the choices teenagers makeThere is no way to legalize marijuana for adults without making it attractive to adolescents - Ed Gogek, MD.
This will be a challenging task as cannabis abuse may become a significant source of income for the cannabis industry. The alcohol and tobacco industry aggressively resisted legislation attempting to reduce use, even as evidence was clearly indicating significant harms. When 50% of alcohol sales go to 10% of drinkers, it should come as no surprise that in Colorado, only 4% of cannabis is sold to occasional users, while less than one third of users consume 87% of the cannabis sold in that state. Even after a series of accidental overdoses in children, Colorado’s health department faced considerable opposition when it attempted to curtail edibles in 2014 amid an industry outcry. Cannabis-infused edibles reportedly make up 45% of the sales and is growing at a rapid pace.
Does legalization increase use?
Many believe that prohibition has failed when considering the many social ills that arise from fuelling the illegal drug trade and abusive prosecutions, and yet, there is historical evidence that suggests prohibition may have been effective in curbing useThe opium wars in China are a good example of the consequences of drug legalization. In 1836, the Emperor of China held a series of Opium Debates between those favoring legalization and those favoring further suppression of opium. Legalizers claimed the real issues with opium were organized crime and argued that legalizing opium and taxing it would generate huge revenues. The British finally forced legalization on the Chinese government in 1858 and the end result was disastrous. At its’ height, it is estimated that over a quarter of the male population was using the drug, a problem which required the brutal suppression of a communist revolution to eradicate in 1949. Another example is alcohol prohibition in the United States in the early twentieth century. While we cannot argue the fact that it fueled organized crime, it also resulted in reducing its’ use and death by cirrhosis by two thirds. of alcohol and opium.
Whether or not legalization will increase use is still up for debate. Several studies in the United States strongly suggest use among teenagers will increase with legalizationAccording to one study, between 2005-2011, rates of teenage use went up 33% in medical cannabis States, while it only went up by 6% in States without these laws., at least in the short-term. SAMHSA data indicates that cannabis use among people over 12 years old has increased from 6.2% to 8.4% between 2002 and 2014 and is now the #1 drug for which U.S. teens seek treatment, and the #2 drug, after alcohol, for adults. According to the National Epidemiologic Survey on Alcohol and Related Conditions, the prevalence of cannabis use has doubled in the United States since the adoption of medical cannabis legislation in the late 1990s and nearly ⅓ of users manifested a cannabis use disorder. In Colorado, data is also showing that legalization is creating other serious problems.In 2011, nearly one in four High School students admitted to current use of cannabis, averaging three times the national average
Between the years 2008/2010 and 2010/2012, current use of cannabis rose by 39% among High School students (grades 9-12) and by 50% among Middle School students (grades 6-8)
Chronic pain has been described as an “epidemic” since the introduction of medical cannabis legislation where over 90% of medical cannabis prescriptions are made out for chronic non cancer pain, a highly subjective qualifying condition and 70% of medical cannabis prescriptions are made out to men between the ages of 25 and 34 years, the demographic most likely to have addictions. When in reality, the majority of chronic pain sufferers are women who are more likely than men to seek medical care for chronic pain. Also, the most common ages for chronic pain in men are the late sixties
A 2014 study by the Colorado Department of Public Health found that Colorado’s adult rate of cannabis use was twice that of the rest of the country, and one third of these users reported daily use and nearly one fifth reported driving stoned
A 2014 survey showed a slight majority of Colorado voters were unhappy with the decision to legalize the drug

The risks of diversion:
Drug diversion is best defined as the diversion of licit drugs for illicit purposes. It involves the diversion of drugs from legal and medically necessary uses towards uses that are illegal and typically not medically authorized or necessary.
It is difficult to speculate precisely the extent diversion will take when cannabis legalization comes into effect, but this is a necessary exercise that we must undertake to fully prepare ourselves for future problems.
According to a study in an outpatient substance abuse treatment clinic in Denver in 2011, 48.8% of adolescents reported getting their cannabis through diversion from a person with a medical marijuana license. This correlates with data on diversion with pain relievers, where 54% of people get the drug through diversion from friends or family.
Brick and mortar sales (dispensaries and Provincial alcohol outlets) and personal cultivationPersonal cultivation may look like a reasonable approach from the outset, but again, cannabis is not like alcohol or tobacco. It’s not simple to grow and cure tobacco or turn out a quality alcoholic beverage that’s better and cheaper than you can buy at the store. Cannabis is a weed and someone with little experience can produce a world class strain. A fully grown plant takes 3-4 months to mature and can generate up to a 1 pound of cannabis. As with pain relievers, it runs the same risk of having a substantial portion of “leftovers” that could generate substantial income. both carry a risk of diversion from licit and illicit sources and will be particularly difficult to regulate and enforce.
Oversight and education to prevent diversion and misuse will continue to be tools at our disposal, as they have been for generations, but their efficacy is limited.
Furthermore, cannabis is unlike alcohol or tobacco products that have remained relatively unchanged for a century or more. In 1880, less than 1% of the population smoked cigarettes. All that changed when the industry matured and began large scale automated cigarette fabrication and introduced smoother blends that enabled deeper inhalation and better nicotine absorption. Along with clever marketing, smoking prevalence peaked at over 40% in the 1950s.
The cannabis industry is experiencing a similar metamorphosis. Smoking the artisanal 2-4% baby boomer bud of the 1960s is gradually being replaced with a practice known as “dabbing” which uses highly purified products such as butane hash oil (BHO) containing 90% THC or more. We have very little data as to the toxicity, addictive potential or the long term harms of these new concentrates but sales are increasing dramatically, and provide another good reason why we should refuse to accept diversion as a benign reality that we have to deal with.

Weighing the traditional methods
At Doctors for Responsible Access, we believe that cannabis legalization needs to be implemented within a framework that enables the following objectives:
- Reduce cannabis youth diversion
- Gather much needed clinical research data
- Provide educational tools with assessment and patient referral mechanisms for physicians who are unfamiliar with cannabis
We believe the pivotal advantage with legalization lies in the use of standardized cannabis preparations for research purposes. Natural variations in each plant’s potency and structure make it impossible to use the street version of the drug in a controlled and safe manner.
We are aware that the approach taken must be carefully balanced between the extremes of total prohibition and unregulated legalization, both of which carry significant social and health harms. As regulations become too strict, the criminal market will continue to thrive. As regulations become too lenient, the risks of diversion and use-related harms potentially increase. When weighing the traditional options“The price of doing the same old thing is much higher than the price of change” - Bill Clinton that have been proposed so far, it becomes clear they all fall short of delivering on these goals:
- Dispensaries offer advice and convenience at the price of increased risk of diversion and black market influence.
- Selling cannabis alongside alcohol in provincially controlled outlets sends the disturbing message that these substances are complementary intoxicants.
- Personal production offers cost benefits (that could be accommodated through legislation by offering incentives to large consumers of medical cannabis) and reliable strain selection and supply (also amenable as industry matures). Studies have nonetheless shown that the grey market associated with personal production is especially difficult to regulate and enforce.
The Quebec Cannabis Registry and the future of clinical research :
Since Health Canada created a unique and rigorous medical cannabis production and delivery systemThe MMPR regulations, enacted in 2013 by Health Canada, has created a strictly regulated national medical cannabis production and distribution system by way of strict quality control standards and a registered mail delivery system through registered mail, we now have a unique opportunity to efficiently address the issues of youth diversion and the need for large scale cannabis research. This system could serve as the groundwork to elegantly achieve these goals.
Safe and secure as it may be, this system is nonetheless burdened with administrative frictions for patients and physicians at the present time:
Present medical cannabis distribution model in Canada :
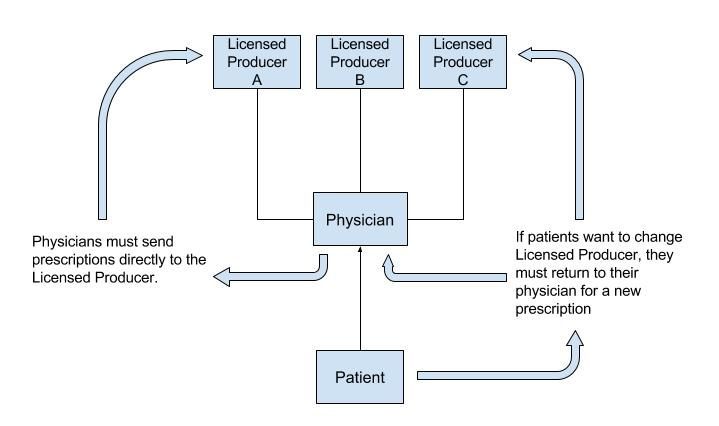 If we were to allow the expansion of this present distribution system to the legal market by way of a centralized platform, all medical and recreational cannabis sold through it would become highly traceable. This, along with tight regulations and education, would add a powerful layer of oversight to discourage diversion to minors. A centralized distribution and monitoring platform would also allow for a more streamlined prescribing mechanism for physicians and enable a more efficient collection system for research data:
If we were to allow the expansion of this present distribution system to the legal market by way of a centralized platform, all medical and recreational cannabis sold through it would become highly traceable. This, along with tight regulations and education, would add a powerful layer of oversight to discourage diversion to minors. A centralized distribution and monitoring platform would also allow for a more streamlined prescribing mechanism for physicians and enable a more efficient collection system for research data:
Proposed medical and recreational distribution model similar to the Quebec Cannabis Registry
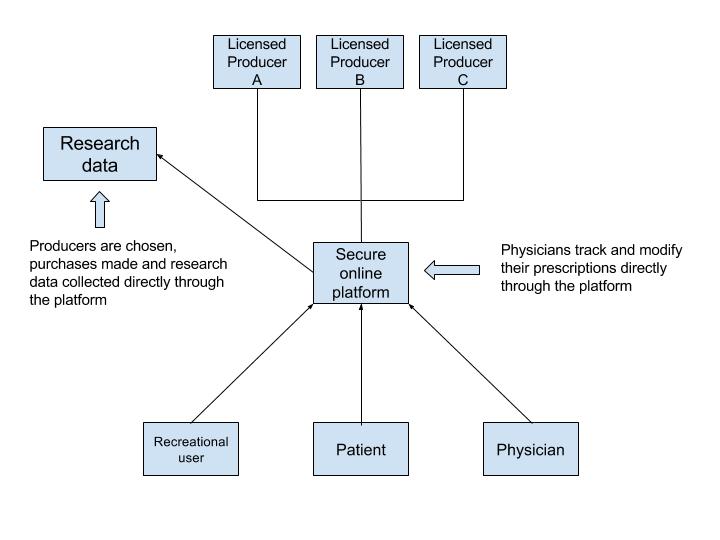 The Quebec Cannabis Registry, offers a model useful to consider. It is a world first for users of medical cannabis and has already begun the process of gathering clinical research data since the implementation of the MMPR. Spreading this system nation-wide and integrating a web-based data capture application such as REDCap™ would give Canada a leading role in cannabis research with the added benefit of reducing the administrative burdens and improving patient access to medical cannabis.
The Quebec Cannabis Registry, offers a model useful to consider. It is a world first for users of medical cannabis and has already begun the process of gathering clinical research data since the implementation of the MMPR. Spreading this system nation-wide and integrating a web-based data capture application such as REDCap™ would give Canada a leading role in cannabis research with the added benefit of reducing the administrative burdens and improving patient access to medical cannabis.
This type of platform would give Canada the opportunity to rapidly legalize cannabis in the form of a prudent scientific study, with the potential added benefit of promoting compliance with United Nations Drug Control Treaties.
After careful analysis, we at Doctors for Responsible Access believe this type of solution, involving strict regulations and innovative technology could help pave the way for a safer and more predictable long term outcome to cannabis legalization.
